Carolina scientists developing contraceptive that stops sperm in its tracks
University of North Carolina Eshelman School of Pharmacy engineer ultra-potent sperm-binding monoclonal antibodies as option for affordable, non-hormonal female contraception
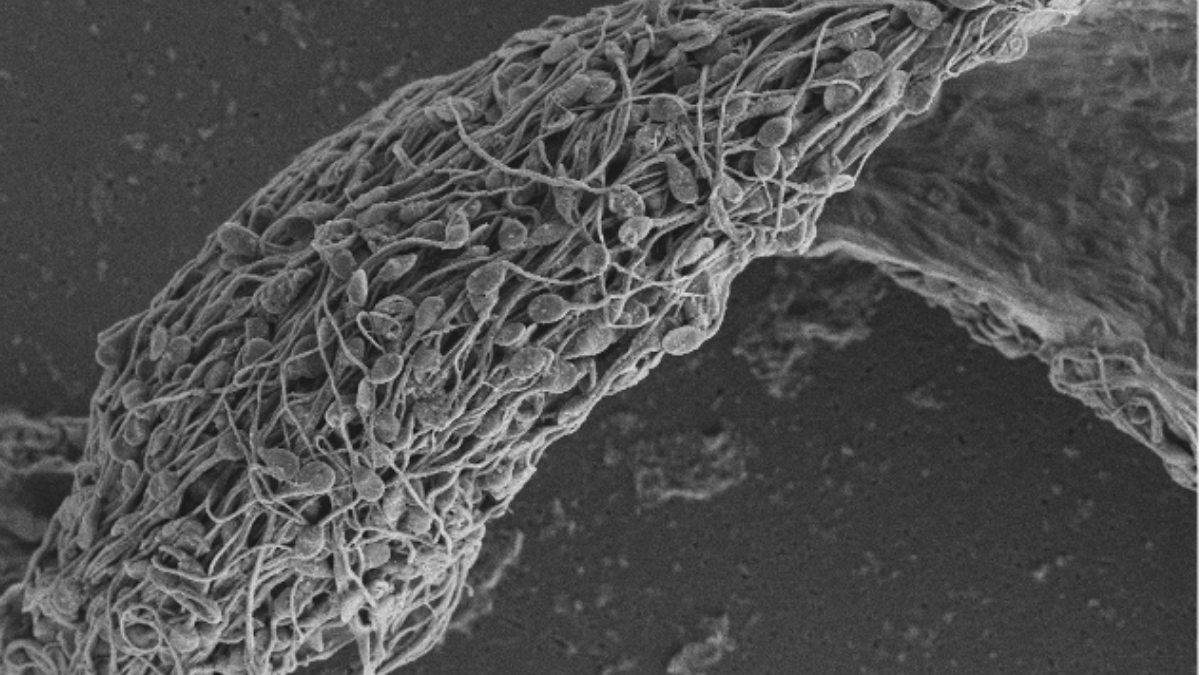
Scientists at the University of North Carolina at Chapel Hill are using the precision targeting of monoclonal antibodies for a new type of female contraception.
Monoclonal antibodies are known for their ability to fight off invading germs and are used to treat and prevent everything from cancer to COVID-19. Scientists are now looking at a new mission for antibodies: immobilizing sperm before it can reach an egg.
Carolina researchers have engineered ultra-potent antibodies that, during animal testing, effectively trapped and blocked more than 99.9% of human sperm. The promising study results published in Science Translational Medicine suggest contraceptives based on antibodies may offer women a non-hormonal option to prevent pregnancy.
“Many women avoid hormonal contraception because of real and perceived side effects,” said Samuel Lai, professor in the Division of Pharmacoengineering and Molecular Pharmaceutics at the UNC Eshelman School of Pharmacy.
These effects can include irregular bleeding, nausea, depression, weight gain and migraines. And for some women estrogen-based hormonal contraception can be harmful.
“There’s a major unmet need for alternative, non-hormonal contraceptives for women,” said Lai.
Antibodies as line of defense
Nearly half of all pregnancies in the United States are unintended, and Lai is among scientists across the country who are advancing the idea of using anti-sperm antibodies for contraception.
“We were inspired by infertility that occurs in some women who develop antibodies against their partner’s sperm,” said study first author Bhawana Shrestha, a doctoral student in the Department of Microbiology and Immunology at the UNC School of Medicine and graduate research assistant at the school of pharmacy.
The antibody they’re testing was isolated from an infertile woman and targets a unique surface antigen present on human sperm. When it’s added to sperm, the sperm quickly clump together.
“Using our highly multivalent IgG platform, we engineered antibodies that were more than 10 to 16 times more potent at agglutinating sperm and reducing sperm permeation through mucus than the best-known antibody,” she said.
Researchers explored the effect of antibodies in sheep, which have reproductive tracts similar to human females. At a high dose of 333 micrograms of antibody, both naturally occurring antibodies and the newly engineered antibodies, effectively stopped all human sperm motility, and at a low dose of 33.3 micrograms, the modified antibodies, but not the original ones, trapped 97% to 99% of sperm.
Next step: clinical trials
But monoclonal antibodies are known as expensive drugs, which puts their usefulness as an affordable contraceptive up in the air.
However, researchers believe that by increasing the potency, much lower doses of the multivalent antibodies may be needed for effective contraception.
“We think these second-generation molecules will provide not only greater potency but will translate to lower costs that make the approach cost-effective,” said Lai.
Mucommune, a startup spun out of the Lai Lab, has licensed the molecule for development of an antibody-based contraceptive. The company will focus on safety and manufacturing to prepare for human clinical trials that could start in 2023.
The team is working on incorporating the antibodies into an intravaginal ring that steadily releases the antibodies, or a dissolvable film placed in the vagina where it spreads antibodies before sex.
“By avoiding exogenous hormones and creating a women-controlled contraceptive method, we believe the antibodies developed here could meet the contraceptive needs for millions of women, help to reduce the number of unintended pregnancies and alleviate the health care costs of unintended pregnancies which some estimate to be in excess of $20 billion a year,” Lai said.
The study team includes researchers from the UNC-Chapel Hill, University of Texas Medical Branch, Boston University School of Medicine and Mucommune, LLC.
The National Institutes of Health, Eshelman Institute of Innovation, the Packard Foundation for Science and Engineering, the National Science Foundation and the PhRMA Foundation funded the study.


